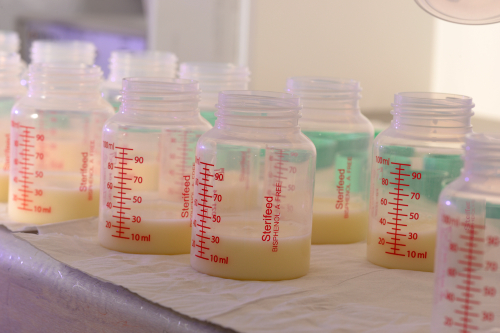
Receiving Donor Milk
Breastfeeding has long been recognized by the World Health Organization as an essential part of newborn care, providing the best source of nutrition, protection against infection, promoting closeness and bonding.
Human milk is especially critical for premature babies, low birth weight, sick infants or where there is insufficient mother’s own milk. Human milk banks can offer safe screened donor human milk as an alternative to infant formula.
In the UK, NHS and nonprofit milk banks adhere to the National Institute of Clinical Excellence Guideline (NICE) for the safe running of milk banks. This means all donor human milk from these milk banks is rigorously screened and from a single donor ensuring full traceability.
Protection From Infection
Donor breastmilk is the preferred alternative to infant formula (or artificial milk). This is because donor breastmilk still contains many of the protective factors (such as immunoglobulins) which help protect premature babies from infection and are not present in formula which is prepared from cow’s milk.
Protection From Necrotising Enterocolitis
Necrotising Enterocolitis is a serious gut condition which mainly affects premature babies. Babies who receive breastmilk either mothers or donor, are at a significantly lower risk than those who receive formula. The reason for this remains unclear although there is evidence to support this.
Easier to Digest
A preterm baby’s intestine is very immature and can digest and absorb breastmilk more easily than formula milk. Premature babies are fed small amounts of breastmilk to help their gut mature and the volumes fed are increased gradually. This is also true for babies who have had surgery on their gut.
Donor Human Milk at Home
For a number of mothers, establishing breast feeding may be challenging, with clinical support, some milk banks may be able to offer a little milk as a “bridge to breastfeeding” to support you. This can be discussed with your health professional and local milk bank.
Where breastfeeding is impossible due to health reasons or medications, some milk banks again may be able to offer donor human milk as an alternative to formula for a short period of time. This is often dependent on supply at the time, this can be discussed with your health professional and your local milk bank.
SPONSORS

Labcold

Savant

Sterifeed

Versapak
UKAMB supports non-profit milk banks by assisting them to fully implement NICE Guideline and to provide safe, screened human donor milk, fully track and trace compliance across the UK and Ireland. UKAMB also recognizes the responsibility and duty of care of milk banks in ensuring donors, donor's infants and recipients are protected from harm by donating or receiving donor human milk.